Recently I have been itching to dip my hand back into life at the hospital. It all started when I attended the annual meeting of the hospital foundation, of which I am a past member. I saw all the fantastic things that have happened in the seven years since I last set foot in the hospital, as well as the great things they have on the horizon. It has reignited my desire to take part and contribute to the hospital’s wellbeing again.
As I discussed my thoughts with the foundation leader, I mentioned that I would love to see the new emergency department (ED), which was completed last year. After I had been retired for four years, I was invited to the groundbreaking ceremony for the new emergency department. I attended and was excited to see the plans for the new ED.
Our little town of 40,000 people has an emergency department that sees 45,000 patients a year and had outgrown its small facility. The new ED has more than doubled its size. My wife and I toured the new facility, and I was blown away by the advancements that had occurred in just the last seven years. I told our tour guide, the director of the emergency department, this tour makes me want to return to practicing medicine. I felt excited again. Here is what I saw.
The Waiting Room
We started our tour in the waiting room of the emergency department which was now double the size it was when I was practicing. What used to be a room to wait your turn to see an ED doc, was now an extension of the emergency department.
There was a nurse assigned to the waiting room! Her job was to triage the patients and begin appropriate treatment before they even get seen by the doctor.
If they are having chest pain, they get a stat EKG. If it showed the patient is having a STEMI (ST – Segment Elevations Myocardial Infarction) the patient is shipped immediately to the heart center in the next town; bypassing our ED completely. Our hospital doesn’t have cardiac surgical capabilities so let’s not waste time sitting here. Time is muscle!
When I was practicing, the ED was just starting a program to treat heart attacks with the same rush to care we were using for trauma victims. Someone who walks into the ED with chest pain now gets the same fast treatment as someone who calls 911 with chest pain.
The nurses have standing orders to give antiemetics to those who were vomiting, to order appropriate lab draws and x-rays so they would be ready by the time the patient got to a physician. There are many other things that have improved by simply placing a nurse in the waiting room to monitor and evaluate the patients earlier.
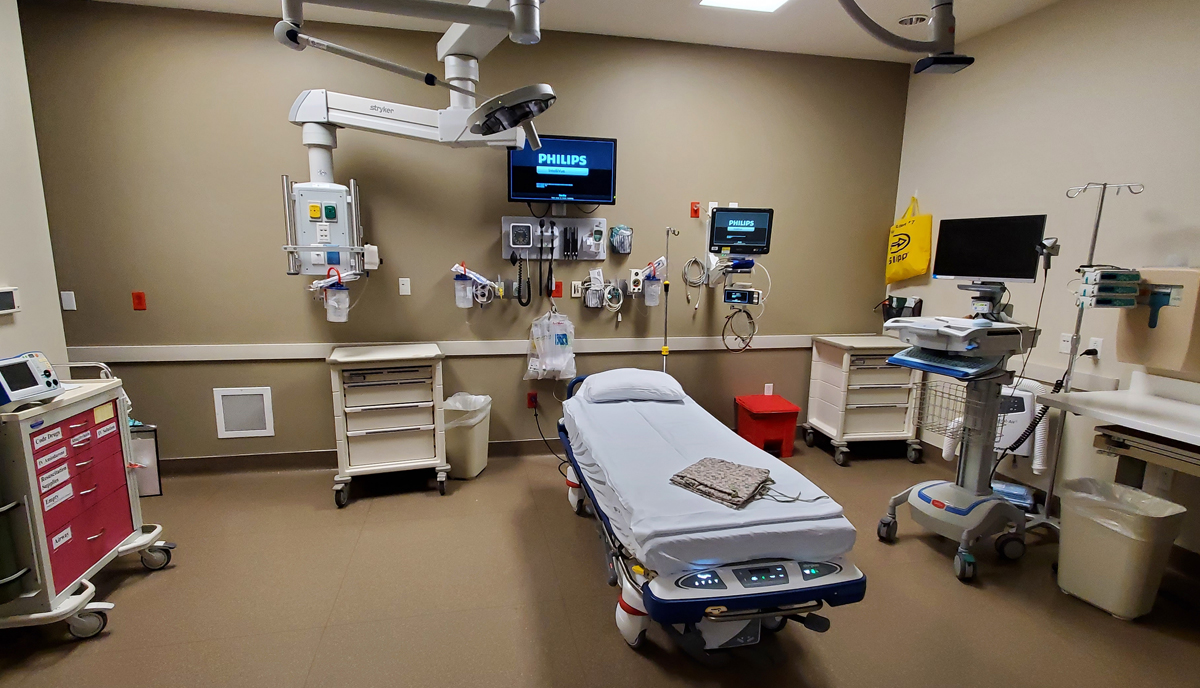
The New ED Rooms
The new rooms are such an upgrade from the rooms I was using when I saw my last patient here at the end of 2015. All the supplies are in carts with wheels so they can be moved in and out of patient rooms to be restocked. It is so much more efficient to roll the cart to the stock room than to bring the stock to the ED rooms.
Several rooms were negative pressure rooms where I believe we only had one or two before. There were two locked in security rooms for mental health emergencies, with many other rooms set up to be back up mental health rooms. These additional rooms have all the medical equipment along the back wall with a garage door that can be lowered to isolate the equipment from the patient in crisis if the main psych rooms are full.
The two large trauma rooms are set up with the tubes going to the patient coming out of the ceiling, instead of from a rolling stand or the wall. This gives easy access to the head of the bed. The days of dancing around the lines and tubes to get to the head of the bed for airway control are over. Now there is clear access around the entire patient.
In keeping with the multi-purpose room concept, these large trauma rooms are also set up with wall attachments, such that when an urgent need occurs, four patients can use this one room. The two trauma rooms can convert into eight patient areas in a mass casualty incident.
There were still a few of the old rooms that were left as they were before the expansion, allowing me to easily see the transformation. The old rooms are much smaller and not as efficient, or as versatile, as the new rooms.
The halls are designed to have extra beds in designated places for overflow. Now the number of patients that can be handled in the ED is much larger than the number of visible rooms.
Technology
The first thing I noticed when we walked into the department was the giant television screens with all the patients referenced. At a glance there was so much information available about each patient. A quick look at one of the two screens will let the doctor know that lab or x-ray results are back, who needs to be seen by a doctor, who is waiting for a room on the floor or has a room assigned, whose Covid test is normal and whose test is positive, and so much more. This was such an improvement from the old board that only told me what room each patient was in.
There was a rolling telemedicine robot available. Now if a consult from a doctor in another city is needed, the consultant can actually see and talk with the patient themselves. This is so helpful for a psychiatric or neurologic evaluation.
Every room has a lighting system on the ceiling outside the door. When a physician or nurse enters the room, the system reads their badge and the correct light turns on letting the staff know, at a glance, who is in each room. If a physicians is needed, they can be found easily without the need to check each room.
The nurses are sitting at stations that face the patient rooms they are attending. And they each have lots of monitors at their fingertips.
Comfort
One of the things I didn’t like when I left medicine was the removal of the things that made it comfortable for the doctors and staff at the hospital. Our doctor’s lounge was taken away, for example, without any warning or consultation with the physicians.
The new ED incorporated specific cubicles for physicians to get their work done; where before we just found a flat spot on the counter to do our charting and dictating. There is also two very nice lounges, one for the nurses and another for the physicians, with an enclosed private outdoor space. It seems like the hospital has changed their stance on making life more comfortable for the physicians.
Also, there are now more restrooms available for both patients and staff. One of the staff restrooms even included a shower.
Helipad
While I was working, I wondered why we didn’t have a dedicated helicopter pad. We had to rope off a section of the parking lot when a helicopter was on the way. Now they have a beautiful lighted landing pad right outside the ED.
When I was doing locums, the little 25 bed hospitals had a good helicopter pad, but our 120 bed hospital did not. When I learned it cost $1,000,000 to put in the pad I realized they need more than just a flat place to land.
It was so exciting to see the improvements that had been made to this 20 year old hospital. The care that went into making both the life of the physicians and the efficiency of the emergency department better exceeded my expectations. I truly believe I would love to work in this new environment. Fortunately, our new graduates have a very nice life ahead of them in medicine with all the new technology and the well thought out setup. It would have been exciting if I could have started my career with facilities like this.
It is truly an exciting time to be a doctor, but I will not be coming out of retirement to see patents again as that ship has sailed. But I do want to get more involved. There are things I can offer as a member of the hospital foundation. I enjoyed my ties on the foundation in the past, and I hope I can contribute again by helping with fund raising to continue to make improvements in the lives of physicians and patients.
I have taken a long enough break from the world of medicine to feel good about contributing again in a new capacity. It is yet to be determined how I will be contributing, but my eyes have been opened to some new possibilities.
Besides getting involved with the hospital foundation, I will continue to coach physicians, which is something that I love, to help them achieve a better live and practice.
Despite all the negative talk about being a physician today, I feel the opportunities are fabulous and this is a great time to become a physician. If you don’t love your life as a doctor, make adjustments so you do. You have the power! There are options.





(Editor: Beware, many incorrect assumptions in this comment> See additional comments)
Seriously, you’re retired clinically and aren’t working and think practicing Emergency medicine has gotten better in the last seven years? This is a parody you writing here right ? Why am confident you wont be signing up to cover Saturday night next week as your ‘contribution” ? If not, Great then ditch your day job and sign up for q6 shifts next month, and be sure to add 4 nights and 3 weekends of course as your don’t want to miss out on all the great developments in practicing emergency medicine . Great new technology? And no mention of the increasingly awful EMR? Nurses in triage? Wow-I don’t realize it was possible/legal ‘ethical to operate without them, but of course many hospitals do. Staffing? Did you say hello to any of the travelers who can’t open the Pixus? Do you meet all the physicians extenders that the attending now has to ‘supervise’? Or say hello to the regional medical director for the national staffing group who also hasn’t seen a patient Ten years ? Oh, when you were working for a small single hospital group back in the day? Oh, they don’t exist any more having sold out to Wall Street years ago (or perhaps you we one of those equity patients that sold out back then?) new rooms that can handle four patients ? Sure the more the merrier. Of course, now they needed when you’re boarding twenty patients , including 4 psych admissions wait for a bed in the next state. ‘The halls are designed to have extra beds in designated places for overflow. Now the number of patients that can be handled in the ED is much larger than the number of visible rooms.’ Whoppee ! Just let my med mal carrier know! I didn’t know whether to laugh or cry reading this piece. You must also believe Liz Holmes is a genuine person and only interested in helping patients? Did you even talk to one of the physicians coming off a shift instead of retired suits like yourself?
John, Thanks for your prospective and I don’t disagree with you. Yes I did talk with the some ED doctors, in fact I talk to practicing doctors all the time as I coach them. I stand by everything I said in the article as there are so many things in medicine that have improved in the last few years. Your response to my thoughts is similar to watching Fox News and CNN right after a presidential address. Both commentators saw the exact same speech but offer opposite opinions. Everything has its downsides and upside and it is up to us which ones we focus on. Every rose bush has both flowers to enjoy and thorns to avoid. I choose to enjoy the sight and smell of the flowers for this article. Other choose to only see the thorns. Our experience in life is vastly different based on which of these approaches we take. I remember working alongside a doctor listening to him rattle off all the bad issues that the EMR caused him that day. He even had tally marks on the board next to him. We both had to work with the same EMR. I’m sure his patients could tell he was having a bad day when he went to see them. I hope you can find some good in your job every day and not only see the thorns. Thanks for your comment.
(Editor: Beware, many incorrect assumptions in this comment> See additional comments)
Look at Dr. Fawcett on line. His premise can I go back is absurd. He transitioned out of clinical medicine to write books, be a financial advisor, advise health care professionals on how to transition to non clinical jobs, reduced scope of practice, or part time with his financial advice etc. He is not an in the trenches dedicated career ED physician. He arranged his life to practice as little medicine as possible. He couldn’t wait to get out
Dear Mark,
Thanks for reading my article and sending a comment to my website. Unfortunately, almost everything you said was incorrect. It seems by your comments that you do not read my material, you simply jumped to conclusions. It was a difficult decision to let your comment go live as it is really not a comment about the article at all, but a slam on me without knowing what you were talking about. But then I thought if you are thinking this after reading my article, others might be as well. So I decided to let the comment go live and correct your misinformation.
Look at Dr. Fawcett on line. His premise can I go back is absurd. Yes that title premise is absurd, I can’t actually go back anymore. The title reflects what I was feeling when I toured the new ED where I practiced. I truly felt “wow, I wish I had all this available when I was working.” During the pandemic I actually did look at going back to help my colleagues during a tough time. Only to find the licensing board would not allow me back in.
He transitioned out of clinical medicine to write books, be a financial advisor, advise health care professionals on how to transition to non clinical jobs, reduced scope of practice, or part time with his financial advice etc. I didn’t transition out of clinical medicine to do any of that. I retired from my private practice of 20 years and began 3 years of part time locums work to help solo small town surgeons survive by giving them a break. In medical school I set a retirement date of age 50. When I reached age 50 I loved my job and didn’t want to retire even though I could afford to. So I transitioned to working less hours and worked a few more years at a bit slower pace doing the locums work. Then I retired fully. I started doing all the things you listed so that I felt I had a purpose during my retirement. I didn’t want to be laying on the beach or playing golf all the time. I wanted to teach other doctors to love their career and have a great balanced family life like I did for 23 years.
He is not an in the trenches dedicated career ED physician. I was never an ED physician, I was a general surgeon/trauma surgeon. I spent 23 years in the trenches and loved my career. It is true that I am no longer in the trenches. But according to your Doximity page, neither are you, since you retired from radiology.
He arranged his life to practice as little medicine as possible. He couldn’t wait to get out. This is not correct and if you made this statement, you have not followed any of my teaching. I suspect this is the first article of mine you have read, but that is an assumption on my part. I did not arrange my life to practice as little medicine as possible. I worked full tilt for 20 years then backed off to half time for 3 years before retiring. I took my share of call and then some. I worked on my days off as well. During my part time years I worked to give lone surgeons in small towns some needed time off. My locums job was to give vacation relief to these surgeons so they could continue to provide care in their small towns. It was a tough decision to leave medicine when I was contemplating retirement. The premise that I couldn’t wait to get out is laughingly absurd.
I coach physicians today to teach them that it is possible to have a great life in medicine, and also to help get their financial situation in good order.
I hope this helps put the article in prospective for you. Touring the New ED really made me feel nostalgic for my years in medicine. It was a great experience and I shared it with my readers.